There are many reasons you may choose to do a semen analysis — maybe you’re planning to freeze your sperm, having difficulty conceiving, or simply wondering about your fertility or male fertility testing options.
This blog post will explain five important things you can learn from your semen analysis, both in terms of your reproductive capabilities and your overall health. It will also cover where to access a semen analysis (whether in a lab or via an at-home sperm testing kit) and how it can help with your family-planning goals.
What is a semen analysis?
A semen analysis, also known as a “sperm count test” or “male fertility testing,” evaluates the quality and quantity of sperm and semen. There are no risks involved with a semen analysis — it’s a non-invasive test performed on semen, typically produced via masturbation.
For the most accurate result, it’s best to avoid ejaculating for 2–5 days before producing a sample for the test. You may also be encouraged to have two separate tests done.
Learn more about how sperm testing and male fertility testing works.
After you provide a semen sample, the semen analysis will evaluate it for qualities including:
- total amount of semen
- sperm concentration (how many sperm)
- sperm motility (movement)
- sperm morphology (size and shape)
Abnormal values may indicate reduced fertility.
What can I learn from a semen analysis?
A semen analysis helps you gain a better understanding of your own fertility, including crucial sperm parameters — metrics that may affect fertility — and overall health.
Sperm testing provides only one indicator of a couple’s fertility. Even if the semen analysis finds abnormal results, your sperm may still be capable of fertilizing an egg and conceiving a child — and vica versa. If you have normal semen analysis results, you may still experience difficulty getting your partner pregnant, since conception requires a healthy sperm, a healthy egg, a healthy uterus, and the right timing.
Here are five things you’ll learn from your semen analysis:
Semen volume
Semen volume is the total amount of semen you ejaculate. The fluids that make up semen comes from sexual glands and organs including the prostate, testicles, epididymis, and seminal vesicles.
Semen volume is important for male fertility because there needs to be enough fluid to carry the sperm to the egg for fertilization. The World Health Organization (WHO) considers a healthy, normal semen volume to be at least 2 mL per ejaculation.
Learn more about what semen is and how it affects fertility.
If you have low semen volume, it may affect your fertility and be a sign of:
- retrograde ejaculation, where the semen is sent into the bladder instead of out of the urethra, resulting in a lower amount of fluid in the sample.
- abnormal hormone levels, such as low testosterone levels.
- anejaculation, where spinal or nerve damage prevents any semen from being ejaculated.
- ejaculatory duct obstruction, where the ejaculatory ducts become blocked by scar tissue, cysts, stones, or other conditions.
In some cases, low semen volume may result simply from collecting your semen sample incorrectly. Make sure to avoid ejaculating for 2–5 days before you produce your sample for a semen analysis, and ensure the entire sample makes it into the sample cup. If you think you made a mistake with sample collection or want a second take, you can do another semen analysis to gain a clearer picture of your fertility.
Sperm count and concentration
Sperm concentration is the number of sperm per mL of semen in your sample. This number, along with your semen volume, can estimate the total number of sperm in your sample (sperm count).
These metrics matter for male fertility because higher numbers of sperm mean that one is more likely to reach the egg for fertilization. If you have a low sperm count, you may be diagnosed with mild to severe oligospermia and have a more difficult time conceiving naturally.
In fact, sperm count is one of the most important factors in determining male fertility. Research indicates that as many as 90% of male infertility issues are associated with low sperm count, and other abnormal semen parameters may be linked to sperm count as well.
According to WHO, a normal sperm concentration is at least 15 million per mL, and a normal sperm count is at least 39 million per ejaculation. Sperm testing is the most effective way of determining yours.
Sperm motility
Sperm motility is the measurement of a sperm’s motion, or more accurately, the measurement of how many sperm are moving and is a crucial parameter in your semen analysis. Sperm need to progress forward — commonly referred to as “swimming” — to reach the egg. If a high percentage of sperm are immotile (unmoving) or moving erratically, it reduces the likelihood that one will successfully reach and fertilize the egg.
WHO states that sperm have normal motility if at least 40% are moving (even if not in straight lines) or if at least 32% display progressive, or forward, movement. They should be moving at a speed of at least 25 micrometers, about half the length of their tail, each second to meet the standards for rapid progressive motility. Moving less than 5 micrometers per second is considered nonprogressive motility.
While reduced sperm motility affects fertility, you may still be able to conceive using assisted reproductive technology such as IUI or intracytoplasmic sperm injection (ICSI), an IVF technique in which one sperm is injected directly into the egg in a lab.
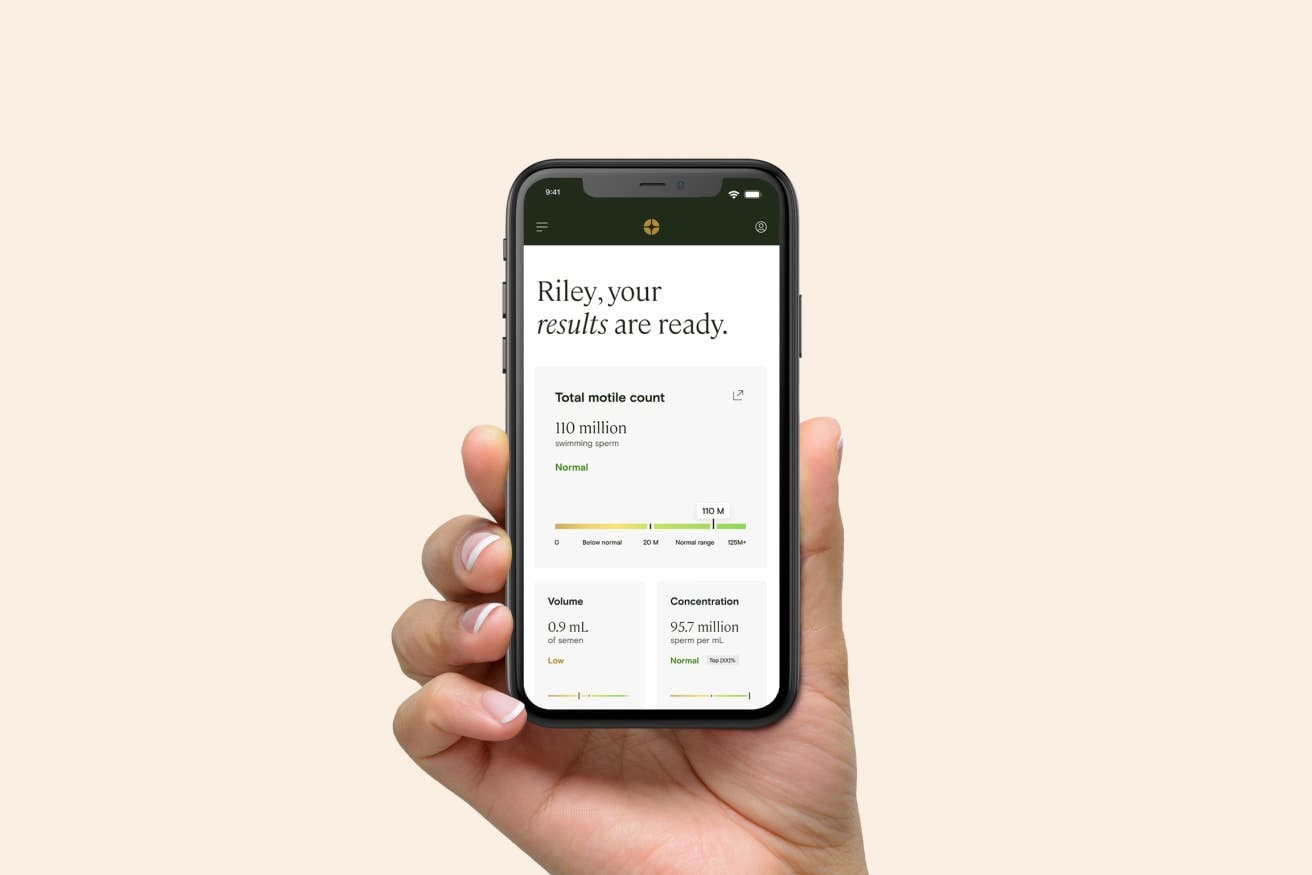
Total motile sperm count
The total motile sperm count (TMSC) is a calculation that reflects your sperm’s quantity and quality. It represents the total number of moving sperm present in your ejaculate sample.
The number is calculated by multiplying your semen volume, sperm concentration, and percentage of sperm motility. For example:
2.5 mL of semen x 18 million sperm/mL x 50% motility = 22.5 million motile sperm
Normal TMSC is 20 million or more sperm.
Since TMSC is based on three factors that affect fertility — semen volume, sperm concentration, and sperm motility — a lower TMSC result suggests a lower chance of conceiving. Research examining semen analyses in infertile couples found that TMSC was correlated with pregnancy rates and was a helpful measure for indicating the severity of male infertility.
Depending on what’s causing your low sperm quantity or quality, you may be able to increase TMSC and improve your fertility through lifestyle changes such as a healthy diet and exercise. One study also found that taking oral antioxidants, such as CoQ10 or other male fertility supplements, was associated with improved TMSC and pregnancy rates.

Sperm morphology
Sperm morphology is the size and shape of sperm, particularly the structure of the sperm head and tail. The form of the sperm affects fertility because abnormally shaped sperm may have trouble reaching and penetrating the egg.
Morphologically normal sperm have an oval head with a cap-like structure, called an acrosome, at the tip, plus a midpiece and long tail. Abnormal sperm forms can include:
- overly large head
- two heads
- no head
- two tails
- crooked tail
- no tail
- bent midpiece
Per WHO, at least 4% of sperm should have a normal shape for a standard semen analysis result. However, it’s possible to conceive naturally even with low morphology.
Abnormal sperm morphology indicates that there may be an issue with spermatogenesis, or sperm production. Still, research indicates that you may be able to improve your sperm morphology by:
- if you smoke, quitting
- If you drink, reducing alcohol intake
- avoiding recreational drugs, including cannabis
- exercising regularly
- reaching and maintaining a healthy weight
- eating a healthy diet
- lowering your stress levels
Benefits of sperm testing
There are many benefits to male fertility testing and sperm testing. Even if your only goal in doing a semen analysis is to freeze your sperm from future use, sperm testing may also give you:
- A better understanding of your own fertility and overall health. A semen analysis reveals the health of your sperm, but it can also help suggest related health issues such as abnormal hormone levels or infections that can affect other parts of your body.
- Clues for an infertility diagnosis. If you have a medical condition that’s affecting your fertility, sperm testing may indicate that something is wrong and put your doctor on the path to determining the issue. Diagnosing the condition after a semen analysis allows you to get treatment and improve your overall health, in addition to hopefully benefiting your fertility.
- Guidance for reaching your family-building plans. If you’re hoping to start or build your family, male fertility testing can tell you if you should be working to improve your fertility, such as by following a healthy diet, exercising, and losing weight or stopping smoking if that’s relevant to you. It can also help direct you toward treatments like IUI or ICSI that may help you and your partner get pregnant.
- Peace of mind: Your semen analysis may be completely normal — a good sign for your fertility and your ability to conceive.
Best of all, sperm testing and male fertility testing doesn’t need to be difficult. You can get started by ordering an easy semen analysis that you can complete on your own at-home sperm testing kit.
When to perform a semen analysis
You can have a semen analysis done at any time to give you a data point about your overall health and fertility. Semen analysis may be most valuable in the following situations.
Semen analysis when you’re trying to conceive
If you are currently trying to get your partner pregnant or thinking about trying to conceive in the near future, it’s a good idea to assess yourself and your partner for fertility with a semen analysis and male fertility testing.
Infertility affects around 15% of couples during their reproductive years, and the male factor plays a role in around half of infertility cases — making male fertility testing an important step in this process. Evaluation is especially important if you’ve been trying to conceive for 6–12 months or more.
Sperm testing if you’re looking to build a family in the future
Evaluating your fertility now can help you assess your chances of conceiving in the near future, and whether you need to make any lifestyle changes to help improve your fertility. You may also want to explore sperm freezing after a semen analysis if you’re not ready to have a family right now.
Male fertility testing to help you improve your fertility
If you want to improve your fertility through a healthier lifestyle or other changes, the first step is to establish a baseline with a semen analysis and male fertility testing.
Semen analysis before freezing your sperm
There are many reasons you may choose to freeze your sperm and preserve your fertility. For one, fertility decreases after around age 40 in people with sperm, so freezing your healthy sperm at a younger age may help you conceive in the future.
Since certain medical treatments, such as surgery and radiation for cancer, may cause infertility, it’s important to freeze sperm before these treatments. This can preserve your option to have genetic children later on. The same applies to preserving sperm before gender-affirming hormone therapy or vasectomy. Performing a semen analysis before freezing sperm is typically recommended.
Finally, with military service being associated with higher infertility rates due to factors including exposure to chemicals and the risk of injury, you may choose to freeze your sperm before being deployed. Regardless of the reason for freezing your sperm, the process includes sperm testing through a semen analysis.
Sperm testing costs
At a traditional clinic or lab, male fertility testing may cost $250 or more, and prices are often not available online. These tests typically require a prescription, meaning you’ll need to attend a doctor’s appointment or fertility consultation beforehand — adding additional costs.
Legacy’s at-home sperm testing kit costs $295 with no prior appointment needed and offers a comprehensive clinic-grade analysis of your sperm’s morphology, concentration, motility, and total motile sperm count. Additional services from Legacy, such as calls with a fertility specialist, fertility improvement supplements, and cryogenic storage of your sperm, can help you maximize your efforts to improve and preserve your fertility.
People often pay out of pocket for services covering male infertility. Depending on your provider, though, Legacy’s at-home sperm testing kit may be covered by your insurance.
Legacy’s at-home sperm testing kits
If heading to a lab is holding you back from doing a semen analysis, Legacy has you covered with at-home sperm testing kits that let you a semen analysis from the comfort of home. Simply order our at-home sperm testing kit, collect and mail back your sample, and receive a report with the results of the semen analysis in less than 2 business days.
Legacy’s semen analysis covers all the crucial sperm parameters: sperm concentration, motility, and morphology, along with semen volume. It can even include a DNA fragmentation analysis, an evaluation of sperm’s genetic health, for deeper insights into your sperm quality.
The analysis has been clinically validated, meaning it’s been shown to achieve comparable results to in-person testing. Conducted in CLIA-certified labs by a team of experienced scientists, all results are reviewed by our medical staff. With this option, you can rest assured that you’re getting accurate results that will help you make informed choices about your fertility.