When it comes to getting pregnant, sperm is half the equation.
Testing from home gives you the power of data in your hands (literally). Start here for more information on sperm testing and improving sperm quality to help you grow your family.
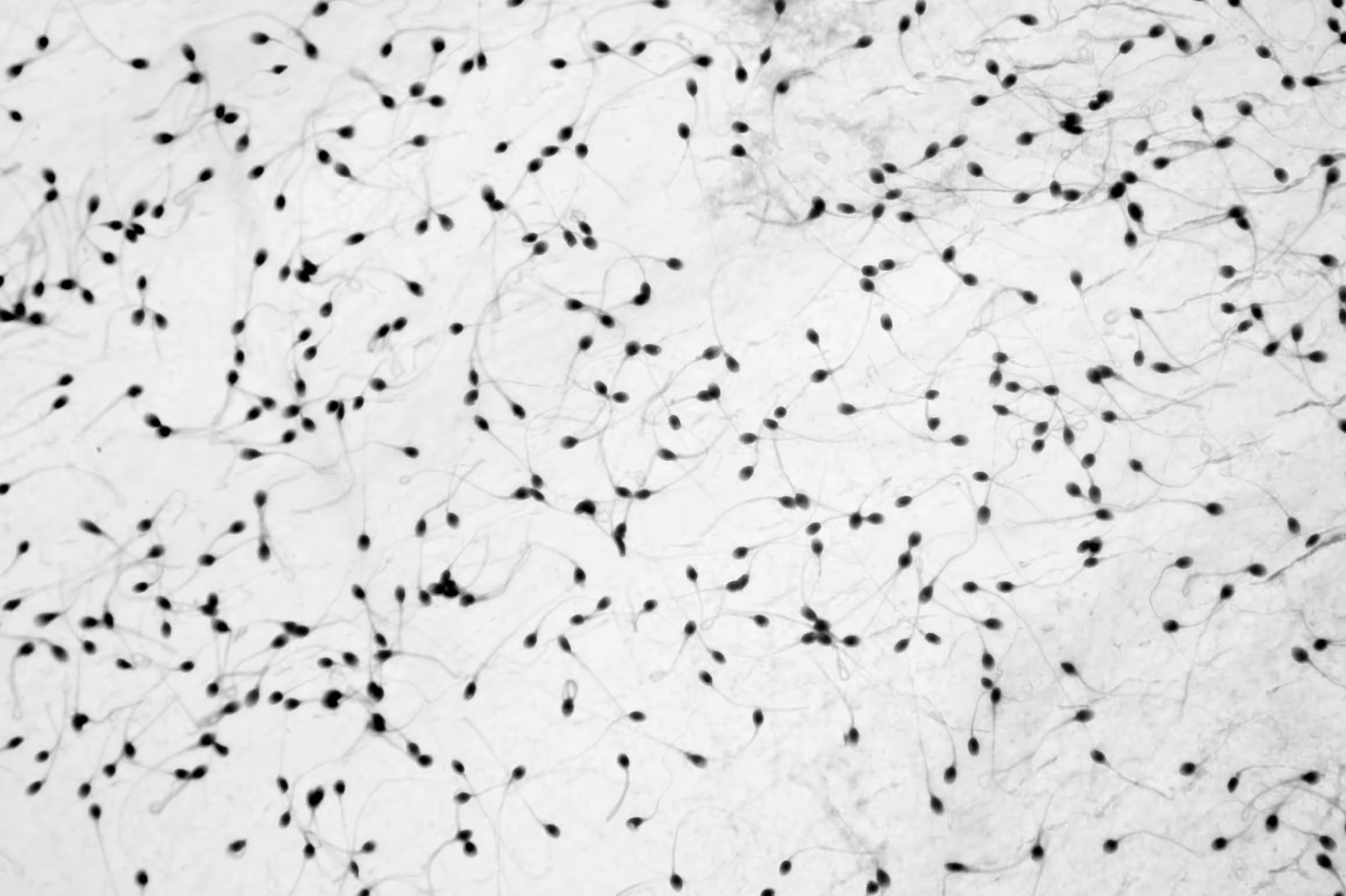
A small cell with a big role
Issues with sperm account for half of all cases of infertility. Sperm quality affects not only whether you’ll be able to conceive, but also the health of the pregnancy and the future baby.
About 1 in 10 men have sperm health issues, and most have no idea. Age, genetics, and lifestyle all contribute — but even young, healthy guys can have issues with their swimmers.

Sperm are on a downswing
Male fertility has declined over 60% in the past 50 years, thanks to our environment and our less-than-fertility-friendly lifestyles. Plus, sperm quality declines with age — about 1% year over year — making it harder to have healthy kids later in life.
Bottom line: if it’s taking you longer than you’d hope to get pregnant, you’re not alone.
But you can take control
You’re producing brand-new sperm every 72 days. If you optimize your lifestyle now, you could be making your healthiest sperm ever in just a few months.
That’s why proactive sperm testing can reduce the chance you’ll need IVF or other fertility treatment to get pregnant. It’s time to empower yourself with information.
Sperm testing is easier than you think
(And we’ve made it even simpler for over 30,000 hopeful parents.)
Everything is easier from home
Our state-of-the-art mail-in kit lets you get a clinic-grade semen analysis without the clinic. That means no collection room or worn out porn — you can test from the comfort of the couch.
From checkout to lab in less than a week
We’re 10x faster than a traditional clinic. Test your sperm on your own timeline — you don’t need to try for 12+ months or get a doctor’s order first.

The info you need to get pregnant faster
Legacy’s sperm testing report helps you understand your chances of conceiving the “old-fashioned way” and includes personalized recommendations for improving your fertility.
Advanced sperm quality testing
Legacy is the only at-home service that offers sperm DNA fragmentation testing to give a deeper insight in cases of pregnancy loss, infertility, or advanced paternal age.
“The whole experience has been awesome. My wife and I are later in age and finally want to try and have a child. The Legacy team are true to their word. Got my kit, followed the easy instructions, sent it off, and like clockwork got my results the next day. Quick, fast and easy! I'm so confident that we will conceive, thanks to Legacy.”
“What sets Legacy apart from other at-home semen analyses is insights into sperm motility and morphology, which are extremely important but not very commonly tested. The coolest part is you'll get personalized, science-backed recommendations for how to improve your fertility health.”
“Legacy’s team of fertility and medical specialists send reader-friendly sperm analysis reports that explain the diagnosis, treatments, and lifestyle recommendations in layman’s terms, instead of incomprehensible medical jargon.”
“Would 10/10 recommend! The reports provided indicate ‘normal’ levels for each data range which is extremely helpful in determining next steps. I am grateful to have found Legacy.”
FSA/HSA eligible
Find what’s right for you
Freezing & testing for wherever you are in your journey
Semen volume
Sperm concentration & count
Motility
Morphology
Sperm DNA fragmentation
Semen volume
Sperm concentration & count
Motility
Morphology
Lifetime access to your Insights dashboard, including your Sperm Score
1 year of storage (renewable)
1 collection kit for 1 sample
Pre-freeze STI kit
Advanced Semen Analysis with DNA fragmentation testing
Ways to save

Insurance coverage
Military & Veteran benefits
Fertility benefits
Learn from the experts
Frequently asked questions
It's a good idea to test your sperm before you start trying to conceive — although anytime is a good time. Our standard semen analysis tests for the main parameters of sperm health (count, concentration, motility, morphology, and semen volume). Sperm testing can identify factors that may make conception difficult, and can reduce the time to pregnancy.
If you are over 35, planning IUI or IVF, or have a history of pregnancy loss, we recommend semen analysis plus sperm DNA fragmentation, a test that measures percentage of sperm that contain damaged DNA.
Once your kit arrives at the lab, your sample will be opened and labeled. The lab scientists will replenish the sperm transport media to ensure the health of the sperm is maintained during analysis.
Next, the sample will be spun in a piece of lab equipment called a centrifuge to separate the sperm from the semen. Once sperm is concentrated, the lab scientists load a slide containing a portion of the sample into the computer-assisted semen analysis (CASA) system. This will report on sperm count, concentration, and motility (the percentage of sperm that are moving or "swimming"). Sperm morphology, the size and shape of sperm, is evaluated manually by an andrology scientist with a high-powered microscope.
If you choose to complete sperm DNA fragmentation analysis, that's performed using the Halosperm sperm chromatin dispersion technique. In this technique, a small portion of your sample is exposed to chemicals that denature, or separate, the strands of DNA in your sperm. This allows the lab scientists to assess which sperm contain broken or damaged DNA that could contribute to issues getting or staying pregnant.
Legacy’s at-home sperm analysis is a clinic-grade semen analysis without the clinic. It looks at all the key metrics of sperm health, including semen volume, sperm concentration, sperm motility, total motile sperm count, sperm morphology, and sperm DNA fragmentation.
Many at-home sperm testing options don’t look at sperm motility, morphology, or DNA fragmentation, which are important parameters. We’re also the only at-home sperm freezing option that includes a post-thaw analysis, in which we freeze and thaw a small portion of your sample to assess if it’s a good candidate for cryopreservation (sperm freezing).
Basic Semen Analysis looks at count/concentration and motility
Standard Semen Analysis looks at count/concentration, motility, and morphology
Advanced Semen Analysis looks at count/concentration, motility, morphology, and sperm DNA fragmentation
A sperm DNA fragmentation test analyzes what percentage of your sperm have damaged DNA. This damage can contribute to infertility, pregnancy loss, and poor health outcomes for your future children.
Together with a semen analysis, sperm DNA fragmentation testing provides a more complete picture of your reproductive health and your chances of conception.
Sperm DNA fragmentation is measured as part of our Advanced Semen Analysis.
No, we can assess sperm DNA fragmentation as part of the same kit that tests for the standard parameters of sperm health (count, concentration, motility, morphology, and volume).
The Legacy kit includes:
- The Legacy “vault,” an insulated zippered container that maintains a stable temperature during transportation.
- A sterile sample cup to easily collect your sample from home.
- The sperm transport liquid — a vial of pink fluid — to keep your sample viable during shipping.
- A security padlock to seal the vault + a strip of tamper-proof tape for extra security.
- Free overnight shipping to send your sample to our lab for analysis.
- Access to Legacy’s client dashboard, where you’ll be able to see your results, where your sample is frozen, and more.
The Standard & Advanced Semen Analysis options also include lifetime access to our Insights dashboard, including your Sperm Score and a comparison of your metrics against thousands of clients your age.
Legacy’s semen analysis kit has been clinically validated. Our research team has compared the results of our kit to a conventional, in-person semen analysis and found no significant difference. There is likely to be a slight decline in sperm motility when using mail-in kits because of time spent in transit.
Legacy’s kit includes a sperm transport liquid that, when mixed with your semen sample, keeps sperm alive and healthy during shipment to our lab for testing.
From prep to results, it can take less than a week.
As soon as you order your kit, it will be express shipped to you. You should abstain from ejaculating for 2–5 days before using the kit. You should collect and return your sample on the same day, between Monday and Thursday. Each kit includes free overnight shipping back to our lab.
Your results will be available in your online dashboard within 48 hours of our lab receiving your sample. If you choose sperm freezing, your sample will be frozen immediately.
Yes, you can use frozen sperm for intrauterine insemination (IUI), in vitro fertilization (IVF), or intracytoplasmic sperm injection (ICSI). If you’re doing a fertility treatment cycle, having a healthy frozen sperm sample on hand can be an important back-up plan.