The hormones that drive male fertility

FSH, LH, and testosterone are three main hormones that drive male fertility. An imbalance in these hormones can affect areas from sex drive to sperm production.
Hormones are chemical messengers that help regulate systems in the human body, like digestion, metabolism, mood, stress, and even reproduction. Sometimes, even minor changes in our hormones — and the balance between them — can have an impact on your body’s processes. Here, we’ll cover the hormones that drive male fertility and explore when testing for hormonal imbalance may benefit your fertility. Testing for hormonal imbalances is particularly important when experiencing symptoms of male-factor infertility.
Key takeaways
- Hormones affect many areas of male fertility, from sex drive to sperm production.
- FSH, LH, and testosterone are the three main hormones that drive male fertility, but other hormones play a role as well.
- Hormonal testing checks for imbalances in hormones that may affect your fertility.
How do hormones affect male fertility?
Hormones play a direct or indirect role in sex drive, sexual functioning, sperm production (spermatogenesis), and more. Without hormone levels in the proper ranges, you may experience infertility.
The hormones that drive male fertility
Three hormones are crucial to driving the process of sperm production and, therefore, male fertility: follicle-stimulating hormone (FSH), luteinizing hormone (LH), and testosterone. These hormones are balanced against one another, with an imbalance in one hormone creating an imbalance in another. The right level of all three is necessary for healthy sperm and optimal male fertility. As such, testing for hormonal imbalances is particularly important.

Follicle-stimulating hormone (FSH)
FSH is produced in the pituitary gland, a small gland in the brain responsible for making hormones that drive many crucial functions of the body. This hormone is key to spermatogenesis. It works closely with LH to produce sperm in the testes.
Specifically, FSH is responsible for the function and maturation of the Sertoli cells, which are somatic (non-reproductive) cells in the testes essential for sperm production. Because of the main role FSH plays in sperm production, low FSH can have serious consequences for sperm count and quality. Hormonal testing would help uncover FSH levels, and reveal whether they impact your fertility.
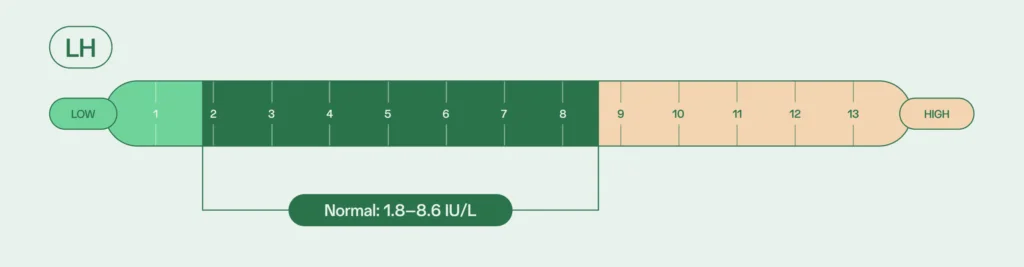
Luteinizing hormone (LH)
Like FSH, LH is produced in the pituitary gland. LH stimulates the production of testosterone that will help support sperm production. As a result, low LH can create a deficiency in testosterone, potentially impacting sex drive as well as fertility.
On the flip side, abnormally high levels of LH or FSH could indicate testicular failure or damage. If spermatogenesis is not proceeding as normal in the testes, the pituitary will go into overdrive, producing more LH and FSH.

Testosterone
If you’re familiar with any male fertility hormones, you probably know at least a little bit about testosterone or “T.” It’s the quintessential “male hormone,” though both male and female bodies produce and require T. Testosterone is responsible for the creation and growth of male sex organs (the penis and testes), and for the development of secondary sex characteristics during puberty, such as muscle growth, body hair, and a deeper voice.
Testosterone is produced within the testicles by Leydig cells. Testosterone is essential for some aspects of spermatogenesis; specifically, it drives the division and differentiation of sperm cells.
Low testosterone is known as hypogonadism and may be caused by age or lifestyle factors. Many people assume having low testosterone levels negatively impacts fertility, but that’s not always the case. Testosterone is not the hormone that actually stimulates sperm production, and many people with low testosterone can still produce healthy sperm. Still, low testosterone levels may affect fertility by causing erectile dysfunction and low sex drive.
On the other hand, increasing your levels of testosterone, such as through testosterone replacement therapy (TRT) or anabolic steroids, will actively impair sperm production and fertility. This is because high testosterone levels decrease FSH, which is essential for stimulating sperm production. Proactive hormonal testing helps in this respect, highlighting abnormal testosterone levels.
Other important male fertility hormones
Along with the three key hormones that impact sperm production, there are other hormones that can impact male fertility as well. While they don’t directly affect spermatogenesis, they still play a role in your fertility and overall sperm health. As such, hormonal testing for these secondary hormones can give you a clearer overview of your fertility.
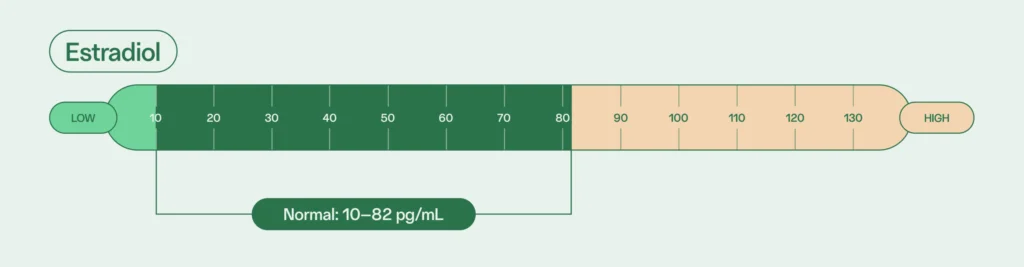
Estrogen
Estrogen is commonly known as a “female” hormone, but it is present both in people with ovaries and people with sperm. Studies show that increased estrogen levels in males can reduce sex drive and decrease sperm concentration and motility.
In people with sperm, the testes produce around 20% of their estrogen. If you have high estrogen levels, you may experience erectile dysfunction and enlarged breasts. Low estrogen levels may lead to a reduced sex drive. Since these symptoms can also be associated with the natural process of aging, it can be difficult to pinpoint this hormonal imbalance.
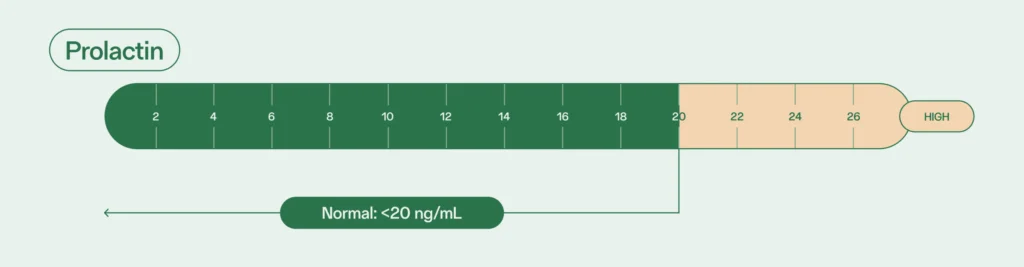
Prolactin
Prolactin is the hormone best known for stimulating breast milk production. However, it also plays several important roles in testicular function and semen production, though its levels are usually low in people with sperm.
An overabundance of prolactin is known as hyperprolactinemia. According to research, this condition is seen in up to 11% of infertile males. It can be caused by pituitary gland tumors, hypothyroidism, and certain medications.
High levels of prolactin have been linked to reduced semen quality. This can inhibit the production of gonadotropin-releasing hormone in the hypothalamus, a ripple effect that causes a decrease in FSH, LH, and testosterone — which, as we know, are key to healthy sperm production. Prolactin is another hormone that is covered in traditional male hormone testing options.
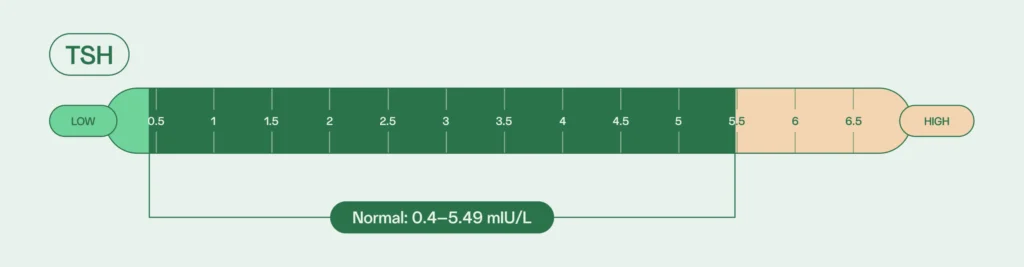
Thyroid-stimulating hormone (TSH)
Thyroid-stimulating hormone (TSH), also produced in the pituitary gland, does basically what it says it does — it prompts the thyroid to spring into action, producing additional thyroid hormones that help maintain the body’s metabolic rate, heart and digestive functions, muscle control, brain development, and bone strength.
If your thyroid is not functioning properly, the pituitary will continue to produce a high level of TSH. Therefore, too-high or too-low levels of TSH in the blood can indicate a problem with the thyroid such as hypothyroidism (underactive thyroid) or hyperthyroidism (overactive thyroid).
Research indicates that both hyperthyroidism and hypothyroidism negatively impact semen parameters like volume, sperm density, motility (sperm movement), and morphology (sperm shape). Although studies have found hypothyroidism has a negative impact on fertility, it is very rare in males, affecting less than 1% of the general male population.
Signs of a hormonal imbalance in male fertility hormones
The symptoms of hormonal imbalance can look similar to the natural effects of aging, so it’s not always easy to catch. Proactively testing for hormonal imbalances is important. Symptoms of a male fertility hormone imbalance may include:
- thinning hair or hair loss
- weight gain or loss
- low sex drive or erectile dysfunction
- fatigue
- depression
- poor semen parameters (low sperm count, motility, and morphology)
What is hormone testing?
Hormone testing for infertility looks for imbalances in your hormones by checking the levels of hormones in your blood. Overly high or low levels of male fertility hormones may negatively affect your fertility or indicate certain medical conditions that could impact your ability to conceive. As a result, undergoing testing for hormonal imbalances when trying for a pregnancy can help identify reasons you may be having trouble conceiving.
If you’re experiencing infertility, you’ll likely be tested for levels of FSH and testosterone, with potential testing of LH and prolactin as well.
Benefits of hormone testing
Hormone testing is a simple way to check for possible causes of infertility. With just a blood test, your doctor may be able to identify conditions harming sperm production or other areas of your fertility.
With the results from male hormonal testing, your doctor may be able to diagnose medical conditions and suggest treatment options to improve your fertility. Alternatively, you may find your best chance of conceiving is with assisted reproductive technology and be able to pursue that option. Male hormonal testing and testing for hormonal imbalances can ultimately help guide your conception journey.
Hormone testing costs
Hormone testing ordered by a doctor may be included in your insurance plan. Depending on your insurance coverage, male hormonal testing and testing for hormonal imbalances may be free or can cost up to several hundred dollars.
You can also use an at-home hormone testing kit. Testosterone testing kits generally cost from $50 to $200 and are less likely to be covered by insurance.
Who should do male fertility hormone testing?
You might want to try male fertility hormone testing if you’re having trouble conceiving or if you have signs of a hormonal imbalance, like thinning hair or erectile dysfunction. Hormonal testing can reveal if these issues are a result of hormone levels and help put you on the path to treatment.
Understanding your fertility: Start with a semen analysis
Your hormones play an essential role in your fertility, but other factors are important too. In addition to testing your hormone levels, you’ll want to get a semen analysis for a more complete understanding of your sperm.
The analysis reveals key aspects of your semen health, including semen volume and sperm concentration, motility, count, and morphology. Each of these factors contributes to your overall fertility.
Better yet, it’s easy to get a sperm analysis. Legacy offers an at-home semen testing kit that allows you to quickly and conveniently test your sperm and receive your results. The test may even be covered by your insurance. With increased understanding of your fertility, you’ll be better equipped to grow your family.
Find what's right for you






