Looking back at the previous year’s fertility trends, and predicting what’s to come in 2021.
In 2020:
The pandemic changed our plans
The COVID-19 pandemic that began in March has changed almost everything about our lives, and family planning is no exception. As health concerns—especially for pregnant people—and financial uncertainties loom, many have delayed their childbearing timelines.
In Modern Fertility’s “State of Fertility 2020: Career & Money” survey, nearly half (49%) of respondents who want children are delaying parenthood, and nearly a third (31%) said COVID-19 has changed their fertility or family-planning decisions. Of those who are waiting to have kids, the primary reasons are financial—60% are delaying because they don’t have enough money saved. Even those who aren’t pausing are feeling the pandemic pressure: 61% of respondents reported that they’re more anxious about their ability to have children right now.

A Fortune survey of would-be parents revealed some of the same grounds for delaying pregnancy during the pandemic. Concerns about health (47%), finances (25%), and COVID-related restrictions (16%) were the top three reasons cited for those putting off expanding their family.
Interestingly, that survey found that some respondents—34%—are actually choosing to move up their family timelines, having children sooner than they otherwise would have. Why? It’s possible that pandemic-era workplace changes, such as remote employment, actually offer a lot of much-needed flexibility for those who hope to have kids (or more kids).
But overall, it’s expected that 2020 will be a “baby bust.” The Brookings Institute predicts the US could experience as many as 500,000 fewer births next year, based on economic studies of fertility behavior and data from past pandemics. This mirrors predictions we reported earlier in the year—that we won’t see birth rates bounce back until 10 or more months post-pandemic (and we’re not there yet).
Virtual and mail-in services became even more important
Many “non-essential” in-person services were suspended this year to stop the spread of coronavirus. Between March and May, fertility care was put on hold based on the guidance of the American Society for Reproductive Medicine (ASRM). Many fertility physicians shifted to virtual consultations, so that patients who were trying to conceive could still plan for their treatment.
And as people self-isolated to stop the spread of coronavirus, many sought testing options that they could complete at home and mail in. The USPS reports that package shipping increased by 50% this year, and that trend included health services.
Examples include LetsGetChecked, a company that offers at-home blood and urine tests for a variety of illnesses and hormones, including an at-home nasal swab for COVID-19. Earlier this month, they reported that demand was up 880% over 2019’s orders. And it’s not all due to COVID tests—competitor Everlywell states that demand has doubled for most of its at-home testing options, including those that detect vitamin deficiencies, Lyme disease, and sexually transmitted diseases.

The fertility space followed suit. Modern Fertility, a female hormone test kit, partnered with fertility clinics early in the pandemic to offer reliable fertility testing from home; their interface allowed customers to send results directly to their doctors. Their CEO reported that, in April of this year, they experienced some of the strongest days their business has ever had.
And our at-home sperm testing kit offers an alternative for those who want a clinic-grade analysis, without actually having to go to the clinic. By August, our order volume was six times higher than it had been at the beginning of the year. “Much easier than going to the REI right now!” one client wrote in a July review.
At-home services mean wider access
The shift to at-home fertility health services has one interesting benefit: It increases access to this type of care, which has historically been difficult to obtain for those outside major cities. A 2017 study reported that 40% of women live in areas with one or fewer fertility practices, and a third had no reproductive endocrinologists in their geographic area at all.
And it’s not just access to testing that’s valuable. Legacy clients, for example, have the option to discuss their results with one of our world-class male fertility specialists, like urologist Dr. Ramy Abou Ghadya, and get expert guidance no matter where in the country they live.
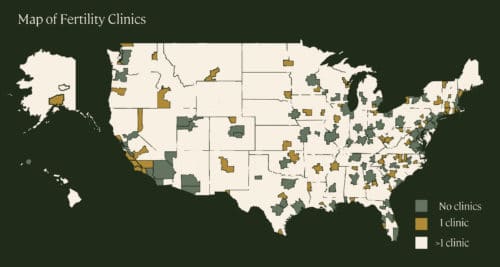
Source: Harris et al, 2017.
There was a focus on freezing
For many of us, this year meant reassessing timelines around relationships and family planning. Single people had a more difficult time dating, engaged people postponed their nuptials, and coupled people were less likely to have a baby right now (see above)—with no clear end currently in sight.
Early in the spread of COVID-19, there was a huge unanswered question: Will infection affect fertility? For men? Women? Both? We are now closer to understanding how COVID-19 affects male fertility: we’re seeing inflammation in the testicles, lower sperm counts, and poorer sperm quality among COVID patients, though we can’t be sure yet how lasting the impact will be. (COVID-19 doesn’t appear to affect female fertility, although a symptomatic infection may dampen your response to fertility treatments.)
As a result of these uncertainties around health, fertility, and timelines, we saw a huge surge of interest in fertility preservation (the umbrella term for egg, embryo, and sperm freezing for later use). At NYU’s Langone Fertility Center, there’s been a 32% increase in women freezing their eggs in 2020. The Colorado Center for Reproductive Medicine, also in Manhattan, reported as early as March—starting just after the first case of COVID-19 was diagnosed in NYC—that they were already seeing a 25% increase in egg freezing consultations.
This has been reported internationally. In the UK, egg freezing inquiries at some clinics are up by 25% compared to last summer. And in Vancouver, Olive Fertility Centre saw cycles increase by 30% year-over-year. Annual metrics for fertility preservation consultations and cycles are up nearly everywhere, despite most clinics being closed for 6–8 weeks early in the pandemic.
We are seeing this trend at Legacy, as well. The number of men who have frozen their sperm with us has tripled since March. Sperm freezing became more important—and popular—as we saw increasing evidence for COVID-19’s impact on male fertility.
While this particular surge is fueled by the pandemic, it comes as part of a long-term trend toward fertility preservation, especially as technology improves and costs drop. According to the Society for Assisted Reproductive Technology (SART), egg and embryo freezing for the future has increased 79% between 2014 and 2018, and the increase is accelerating. Unlike these treatments that require a fertility clinic’s oversight, we don’t have national numbers for sperm freezing—but anecdotally, demand is up as awareness about men’s fertility issues spreads.
We embraced technology as part of the pre-conception process
More than ever, couples who are trying to conceive are utilizing technology, like wearables, apps, and algorithm-based guidance, to get pregnant more quickly and detect issues earlier.
Ovulation tracking tools are one example. Women have been tracking their menstrual cycles for centuries, although the modern method for estimating the fertile window—basal body temperature tracking—was developed by a gynecologist in the early 1900s. Apps, often paired with a thermometer (like Natural Cycles) or a wearable (like the Ava bracelet), make the process nearly error-proof.
In a March 2020 study of Australian women, nearly half were using phone-based apps to monitor their menstrual cycles. The good news? It works. A 2019 study demonstrated that any method of cycle tracking was associated with faster time to pregnancy, even for women who had experienced difficulty getting pregnant in the past.
But as we know, fertility is not merely a women’s issue. On the male side, the Legacy sperm testing kit utilizes technology to proactively address sperm health. Our algorithm incorporates your lifestyle assessment, your semen analysis results, and a specialist’s inspection to give you a comprehensive understanding of your fertility. Your results will be accompanied by personalized lifestyle guidance to help you improve your sperm health parameters on your own.
Traditional advice recommends that couples try to get pregnant for 6–12 months before doing this kind of testing. But time is of the essence when it comes to fertility, and using technology can allow people to get pregnant on their own more quickly, or alert them that they may need help from a fertility specialist—all for less than the cost of a consultation.
Looking forward to 2021:
We’ll continue to see downward fertility trends
We reported last year that the US fertility rate hit an all-time low of 1.72 children per woman in 2019. That decline isn’t all bad. Having fewer children is often the result of wider educational and professional opportunities, especially for women; better healthcare, which means children are more likely to survive to adulthood; and higher contraceptive use that allows couples to plan their families and lowers the rate of accidental pregnancies.
But falling birth rates also point to other trends: increasing parental age and declining male fertility.
In 1972, the average age of first-time fathers was 27. Now, it’s around 31 years old—and nearly 1 in 10 fathers are over 40 at the birth of their first child, according to a 2017 study. There are many influences that lead to having kids later in life; increased educational and professional opportunities come into play again, along with growing monetary insecurity for young people.
While studies suggest that it can be financially, emotionally, and intellectually beneficial for children to have older parents, age is also one of the most important factors in fertility. We know that sperm quality declines with age, that infertility is more likely among couples with older fathers, and that older men are less likely to produce healthy offspring. We also know that there’s a steep decline in egg quantity and quality (or genetic health) for women in their late 30s, bringing the chances of natural conception down to 10–15% per month.
Increasing parental age is only compounded by the declining male fertility rates we’re seeing across the Western world. According to one study, sperm count declined 50–60% between 1973 and 2011; another study found that sperm concentration has decreased by a third in the past 50 years. Sperm motility has declined as well. One group of researchers found that the percentage of men with normal numbers of motile sperm had decreased by 10 points over 16 years.
Why? Experts aren’t entirely certain, but exposure to plastics, toxins, environmental pollution, and radiation; increasingly sedentary lifestyles; and the common Western diet may all be to blame.
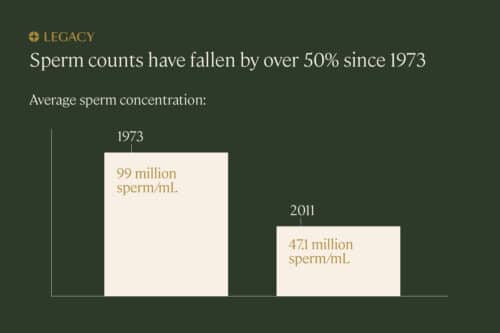
The COVID-19 conundrum
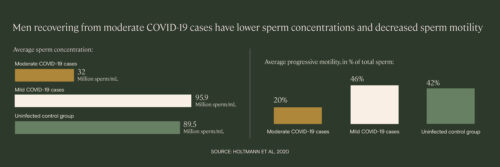
We’re likely to see a significant drop in births for about 10 months post-pandemic, as people wait until they feel safer and more financially stable to grow their families. But we’re also seeing significant impacts of COVID-19 infection on male fertility. One study found that men with moderate COVID cases have, on average, a third of the sperm concentration and half the percentage of motile sperm, compared to uninfected controls.
Since COVID is a new illness, we don’t yet know how long this effect will linger—the longest follow-up study performed so far was 54 days post-infection. But it’s possible that, in addition to the declining male fertility we’ve been experiencing over the past few decades, we’ll soon be seeing a lasting imprint of the pandemic on male fertility.
We’ll reconsider what the modern family looks like, and how it’s built
We’re no longer in a heterosexual male-breadwinner two-point-five-children world. Changing gender roles and wider acceptance of LGBTQ people means that the modern family is changing.
Men are taking more of a role in raising their children than ever before. The number of stay-at-home dads doubled between 1989 and 2012, according to Pew, and is likely to continue to rise. A 2015 BabyCenter survey of millennial dads revealed that 26% of respondents were the primary caregivers for their children, and the majority had at least partial responsibility for many childcare tasks. Today, couples are embracing an egalitarian approach to both their own partnership as well as parenting.
We’re also seeing a rise in families with LGBTQ parents. In 2019, a Family Equality survey reported that 63% of younger LGBTQ people had children or planned on having children, nearly double the number of older members of the community with children. It’s possible that, even if older LGBTQ people wanted children, they simply didn’t have access to—or couldn’t afford—the medical technology (or adoption assistance) necessary to make that happen.
But today, there are more options. Reciprocal IVF, a process in which one female partner donates her eggs to the other so they can both be involved in the pregnancy, is a growing practice. In April, New York—one of the last three holdout states—legalized gestational surrogacy, in a decision that was celebrated by fertility advocates and LGBTQ advocates alike (surrogacy is necessary for a gay couple to have a biological child). Soon after, journalist Anderson Cooper welcomed his first child via surrogate; Anderson is gay, and raising his son as a single dad.
We’re also seeing a new focus on fertility, specifically fertility preservation, for trans people. For example, it’s increasingly common for trans men to freeze their eggs prior to transition, and for insurance plans to foot at least some of the bill. Trans women can also freeze sperm prior to hormone treatment.
We expect that the movement toward a more diverse picture of the modern family, and the modern father, will continue in 2021. Parents of the near future will likely share the playground with single dads, stay-at-home dads, queer parents, trans parents, and more.
We’ll squash fertility stigma—and keep expanding awareness
We’re talking about fertility more than we ever have before.
Over the past few years, there’s been a huge push by physicians to educate the public on their biology, as well as their fertility options. A survey in 2016 found that the majority of both men and women were misinformed about female fertility decline and the impact of age on your ability to have a healthy pregnancy. Our own 2019 survey found that almost 70% of respondents didn’t know that age impacted sperm health. There’s clearly still a gap that needs to be closed, and we predict that we’ll make some progress on that in the coming year.
One thing that helps spread awareness? Hearing people talk about fertility. Historically, it’s been somewhat of a taboo topic. Superstitions and myths around fertility and pregnancy, a societal aversion to discussing “women’s issues,” and the fact that many people struggling with infertility or miscarriage blamed themselves made it a difficult thing to talk about publicly.
That’s changing. Public figures as varied as Amy Schumer, Chrissy Teigen, the Kardashians, and Michelle Obama have gone on record to discuss their experiences with infertility, pregnancy loss, or prenatal difficulties. And on platforms like Instagram and Facebook, support communities have blossomed as more men and women are willing to share their stories in real time, posting images of their embryos, diagnostic results, and pregnancy tests—both positive and negative—under hashtags like #TTCjourney.
It’s happening offline, too. Respondents to the Modern Fertility Career & Money survey, for example, were surprisingly willing to talk about pregnancy and fertility concerns in the workplace—where the stigma against these conversations still has a stronger hold. Nearly a third of women surveyed said they’d talk about fertility treatments, infertility, or miscarriage at work; in addition, 28% would share early pregnancy news, 25% would share that they’re going through the process of egg freezing, and 26% would share when they’re actively trying to conceive.
These conversations are likely to continue into 2021, and we predict they’ll broaden to include less-told stories, such as male-factor infertility, single parenthood, and LGBTQ child-bearing. The more we talk, the more we learn—and the more we learn, the better decisions we can make for our own lives and the lives of our future kids.



