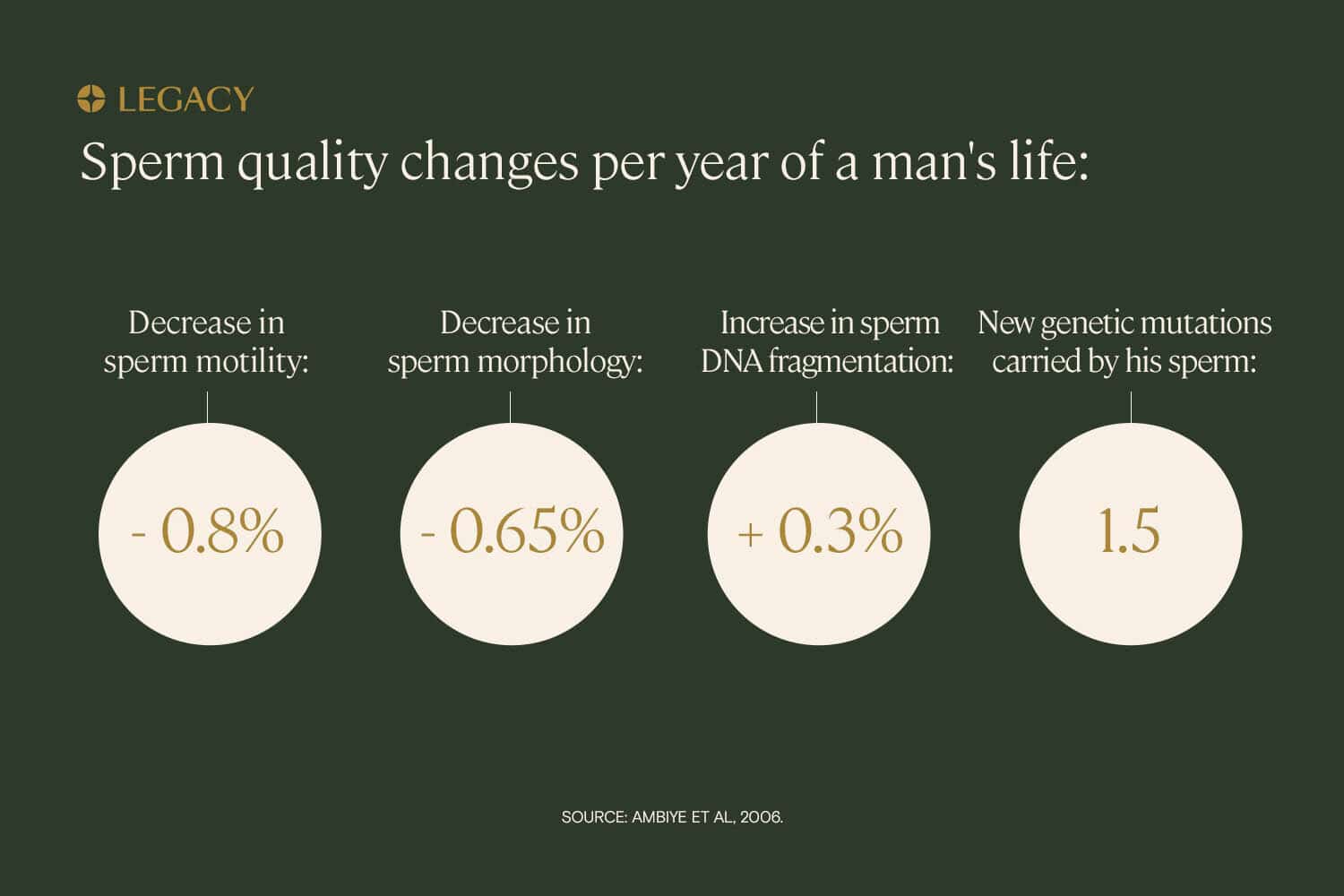
While a person who produces sperm typically does so for their entire life, there’s a measurable decline in sperm count and quality with age. This results in lower pregnancy rates, higher miscarriage rates, and a higher chance of health issues for the offspring of older parents.
Sperm freezing can provide you with more options when it comes to when and how you want to start a family.
Learn more about male fertility and age.