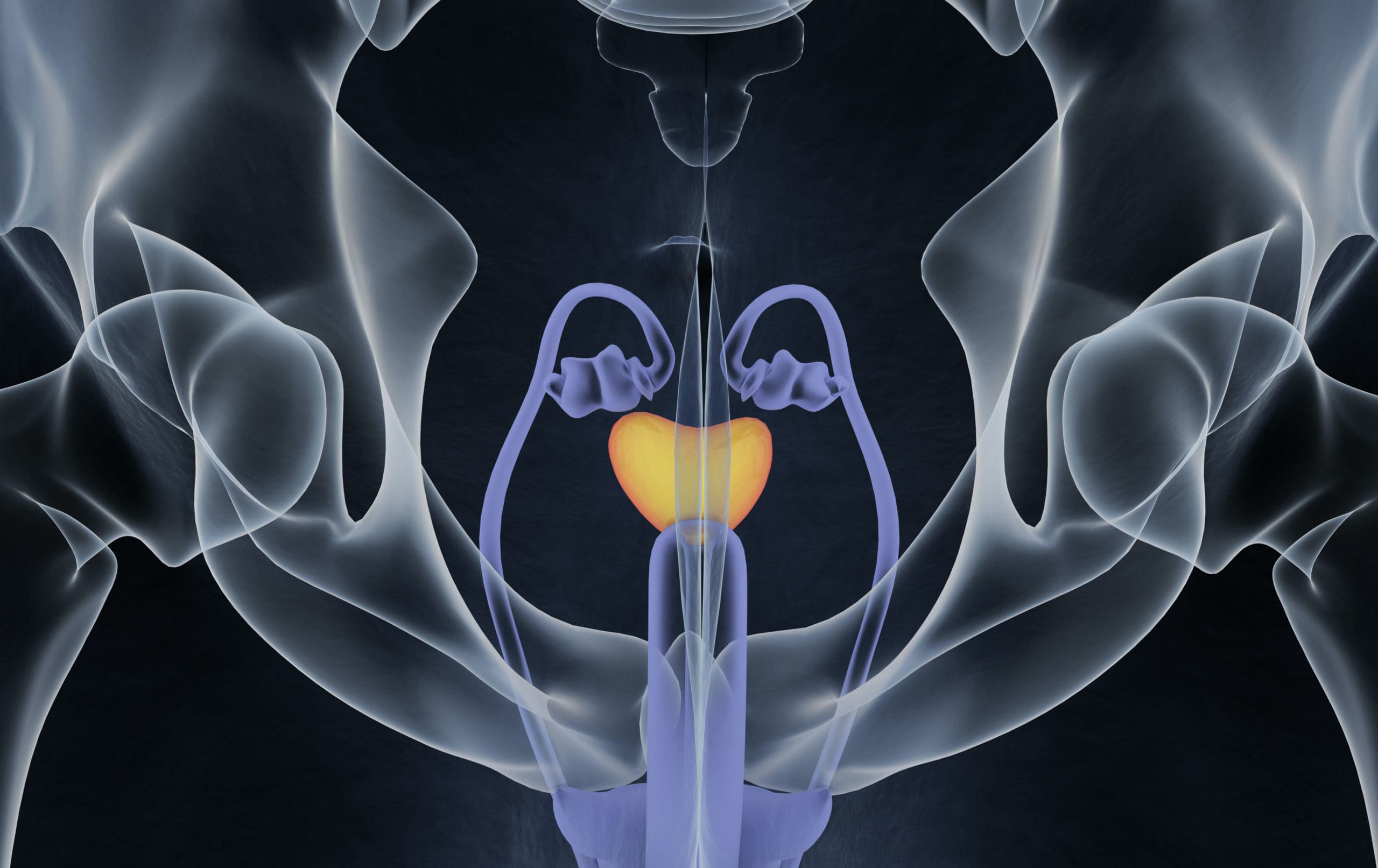
How familiar are you with your vas deferens? These ducts are an integral part of the male reproductive system. Do you know how the vas deferens functions, and what role it plays in your fertility?
First, let’s revisit all the organs that make up the male reproductive system:
- External organs: Penis, scrotum, testes, and epididymis.
- Internal organs: Vasa deferentia (plural for vas deferens, because there’s two), ejaculatory ducts, urethra, seminal vesicles, prostate gland, and bulbourethral glands.
The main functions of the male reproductive system are to:
- Produce, store, and transport semen — containing sperm — from the testes to the female reproductive tract
- Produce and secrete important sex hormones
So, where does the vas deferens fit into this picture?
What is the vas deferens?
As noted above, the vasa deferentia are part of the internal male reproductive system. You may have heard them referred to as ductus deferens or sperm ducts. Essentially, they are tubes that carry sperm out of the testes.
The process begins with sperm production. Sperm production (spermatogenesis) happens in the testes. Healthy men will produce around 50–100 million sperm daily. Once the sperm mature (which takes about 74 days), they’re stored in the epididymis, a structure in the testicles. This is where the vas deferens come in.
There is one on each side of the testicles. One end of the vas deferens starts in the scrotum, attached to the epididymis. The other end connects to the duct of the seminal vesicle inside the body, creating the ejaculatory duct. This then connects with the urethra. The total length of the vas deferens can be up to 18 inches.
The principal function of the vas deferens is to transport sperm from the testes and out of the body during ejaculation. Here’s how it works:
- During arousal, muscle contractions help move the sperm from the epididymis through the vas deferens.
- The vasa deferentia connect to the seminal vesicles, where your body produces semen. There, the semen mixes with the sperm.
- Finally, the semen moves from the ejaculatory duct to the urethra for ejaculation.
This makes the vas deferens pretty vital when it comes to fertility. Sperm must be able to move through them, mix with semen, and exit the penis during sex. Conditions that affect the vas deferens can therefore have a significant impact on fertility.
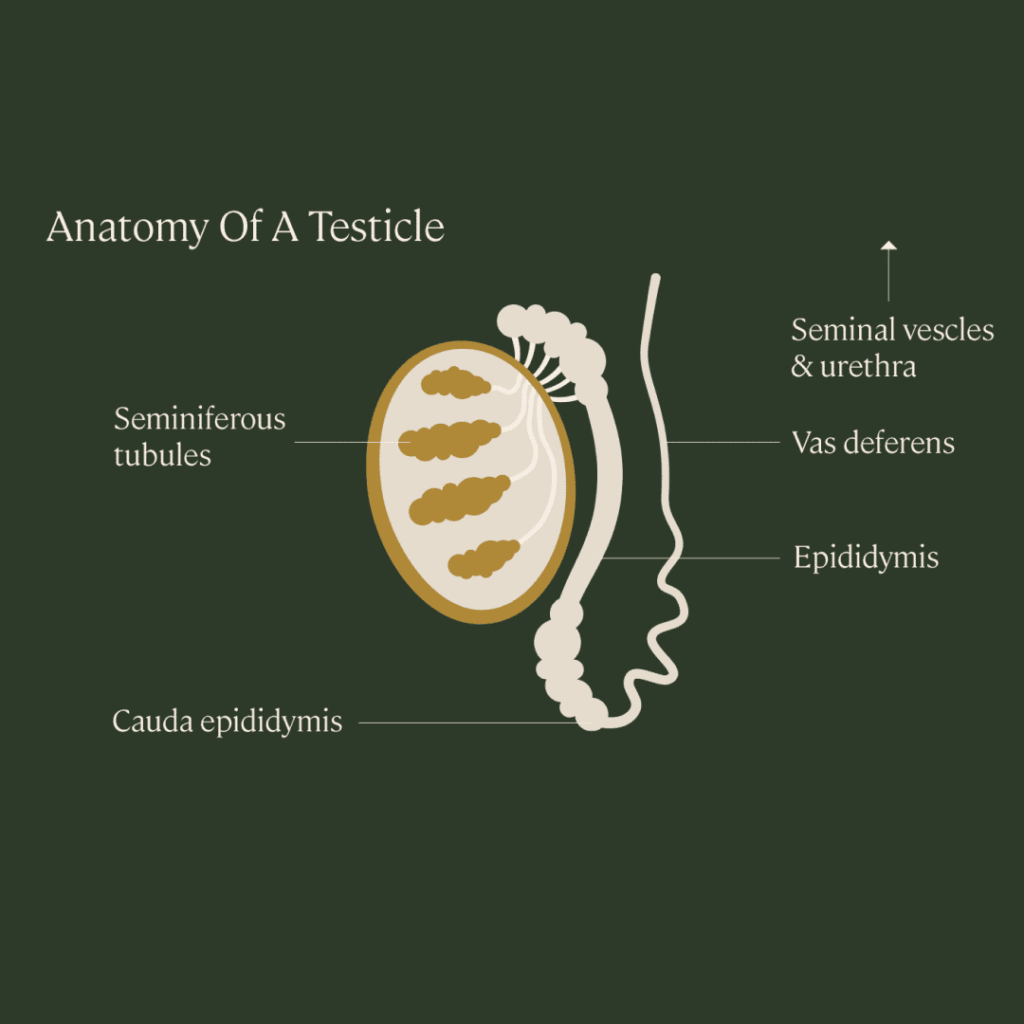
The vas deferens and vasectomy
Some people are familiar with the vasa deferentia because they’ve researched or had a vasectomy. Vasectomy is a form of permanent contraception for people with sperm.
During a vasectomy, the vas deferens on each side of the testes are cut and closed off. This means that you’re still producing sperm, but it has no way to get out of the body. It’s a highly effective form of birth control — over 99.9% effective — that generally doesn’t affect sexual function, hormone levels, or other aspects of reproductive or sexual health.
Vasectomy is not always reversible. We strongly recommend sperm freezing prior to vasectomy, just in case.
Blockage in the vas deferens
The vas deferens can become blocked, preventing the travel of sperm. Some conditions that can cause this include:
- Vasitis: Inflammation and swelling of the vas deferens. Most often, this is associated with having a vasectomy, although urinary tract infections can also cause it.
- Infections such as sexually transmitted infections.
- Spermatocele: A type of cyst that develops above or behind your testicle.
- Testicular conditions such as testicular cancer or testicular torsion.
- Trauma to the testicle area.
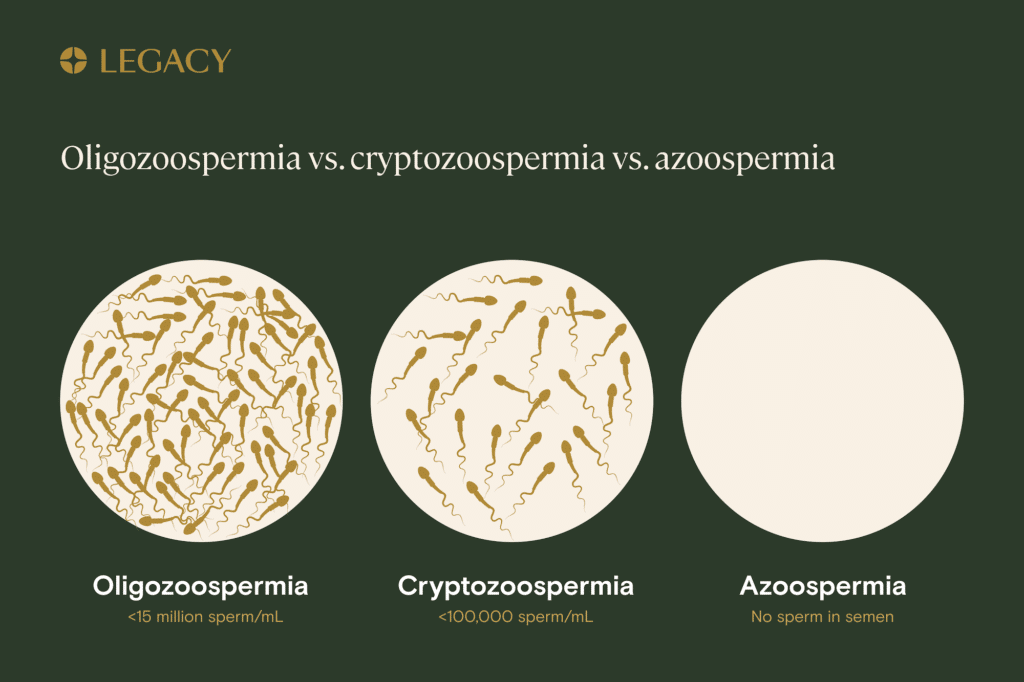
Typically, the way a person will find out that they have a blockage in the vas deferens is via a semen analysis. Their results may find that they have no sperm in their sample, a condition called azoospermia, or may find a very low sperm count, called cryptozoospermia.
Are you missing one or both vas deferens?
In some cases, it’s not a blockage of the vas deferens that’s the problem, but one or both may be missing.
Some people have a condition called congenital absence of vas deferens (CAVD), which means they are born without one or both tubes. More specifically, congenital bilateral absence of the vas deferens (CBAVD) means both vasa deferentia are missing, which is much more impactful in terms of fertility.
Sometimes, CAVD can happen randomly, when the vas deferens do not develop properly before birth. However, it can also be a sign of cystic fibrosis. This genetic condition causes sticky mucus to build up in the lungs and digestive system. Nearly 95% of men with cystic fibrosis have CAVD. Interestingly, some men who are carriers of the gene mutation that causes cystic fibrosis may also have CAVD, even if they don’t have cystic fibrosis.
Many people born without a vas deferens do not know they have this condition until they are trying to conceive. The primary way to diagnose absence of the vas deferens is through a semen analysis. When there is zero sperm in a person’s semen sample, it is called azoospermia. Azoospermia leads to issues conceiving, as sperm is required to fertilize an egg.
Although those without a vas deferens are infertile, they are typically not sterile. Sperm production may still be normal. The sperm just can’t make it to the semen due to the absence of the vas deferens.
Treatment for people with vas deferens issues
Before having any treatment, you will need additional tests to pinpoint the problem with your vas deferens. The type of tests you need will depend on what your health care provider suspects the concern is, and they will talk you through each stage of the process.
If you’ve had a semen analysis come back with reports of very low or no sperm count, a doctor may order the following tests:
- An ultrasound to identify whether you are missing one or both vas deferens, or to spot a blockage
- Urine and blood tests to rule out other issues, such as retrograde ejaculation or hormonal imbalance that may cause male infertility
- A testicular biopsy, a test in which a small piece of tissue is removed and examined to see if sperm are being created in the testes
If your clinician identifies a problem with your vas deferens, there are several treatment options available:
- Medications such as antibiotics can be used to treat infections, reducing the inflammation and swelling.
- Surgery. If a cyst, varicocele, or mass is the cause of the vas deferens problem, a surgeon can repair this and remove the cause of the blockage.
- Testicular sperm extraction (TESE). If you have low or no sperm in your semen (azoospermia), but you’re producing sperm, you may need to have sperm collected directly from the testicles surgically. TESE is helpful for people with CBAVD who are producing healthy sperm, but lack the pathway to get sperm out of the body.
- IVF with ICSI. In vitro fertilization (IVF) is a type of artificial reproductive technique where an egg is fertilized by sperm in a lab. This can be a successful route to conception for men with CAVD following testicular sperm extraction. Sperm collected via TESE will be injected directly into the egg using intracytoplasmic sperm injection (ICSI).
The positive takeaway is if you are having fertility problems due to a blockage of your vas deferens or CAVD, many treatment options are available to assist you on your family-building journey.
Testing your fertility
Many people who have issues with their vasa deferentia — or have no vas deferens at all — have no other symptoms. Therefore, fertility testing such as semen analysis is important to identify and diagnose any potential issues.
Legacy offers easy at-home sperm testing, so you can be proactive about your fertility.