Post-thaw analysis: Why is it important?

Legacy’s at-home sperm freezing kits include a thorough post-thaw analysis. Find out why this service is important and what information it provides.
A post-thaw analysis is a crucial step in the sperm freezing process. It allows lab technicians to evaluate how a semen sample withstands the sperm freezing and thawing process. Not all at-home sperm freezing kits include a post-thaw analysis, leaving out important information on sperm motility and viability. Read on to understand how a post-thaw analysis is conducted, its importance in the sperm freezing process, and what should be expected in the results.
Key takeaways
- A post-thaw analysis is a test that assesses how well sperm survives the sperm freezing process. It gives clients an idea of what their total motile sperm count will be when sperm is ready to be used.
- The sperm freezing and thawing process does result in a slight decline in sperm quality, including motility, but this decline should not affect pregnancy outcomes if the sample provided was within healthy sperm parameters.
- While most traditional clinics do provide a post-thaw analysis when you opt for sperm freezing, Legacy is the only at-home freezing kit that includes this service.
What is post-thaw analysis?
A post-thaw analysis is comparable to a “test run.” It assesses how well sperm can withstand the sperm freezing and thawing process.
The test involves freezing a small sample of semen at the standard -196°C. This is done by an andrologist or embryologist, a lab scientist who’s an expert in working with reproductive materials. Then, the scientist will thaw the sperm using standard protocols and evaluate how many sperm are still viable (alive) and motile after undergoing sperm freezing and thawing.
Without a post-thaw analysis, it’s difficult to estimate how many sperm will be viable when the sample is ready to be thawed and used in the future.
The sperm freezing process
Also known as cryopreservation, sperm freezing involves a number of steps that begin with a semen analysis. This analysis ensures there are enough healthy sperm to freeze and assesses parameters like sperm count, motility, morphology. If sperm can be improved, the sperm freezing process may be postponed until necessary interventions have been made.
The semen sample then goes through processing, which includes “washing” the sperm with a special solution to remove semen plasma and any contaminants in the sample. The sperm is also treated with small amounts of cryoprotectant, a chemical which prevents damage during freezing.
Sperm is then separated into vials and slowly frozen in liquid nitrogen to -196º C, the temperature at which all biological activity pauses. At this point, the sperm is stored or transported in liquid nitrogen banks to a sperm bank. A small portion of the sample is reserved for post-thaw analysis purposes.
The post-thaw analysis process
After a semen sample has been collected and analyzed, a small portion is reserved for the post-thaw analysis. This involves freezing the sample to -196ºC, thawing it at 37ºC (body temperature), and then performing a second semen analysis. This analysis will assess the remaining sperm count and motility, or how many sperm are moving properly.
The post-thaw analysis provides a clear picture of what can be expected when the cryopreserved sperm is ready to be used and is a crucial step to sperm freezing.
Does sperm freezing affect quality or motility?
Freezing and thawing sperm results in a slight decline in sperm count and quality, including a reduction in sperm motility. Research shows that 82–85% of sperm generally survive and remain motile following sperm freezing and thawing.

Storage for over 10 years may cause a slightly more significant drop in sperm count and quality, But a 2019 study found that the slight decline in sperm’s survival rate after sperm freezing made little difference to the pregnancy and live birth rate, with success rates comparable between 6 months of freezing and 15 years.
There have been cases of success with sperm that has been frozen for long periods of time. A 2013 study presents a case in which sperm frozen for 40 years resulted in the birth of healthy twin girls.
The importance of post-thaw analysis
Since a slight decline in sperm count and motility is expected after thawing, a post-thaw analysis gives clients and their doctors a more realistic idea of what can be expected after sperm freezing when it comes time to use it.
Fertile men produce at least 20 million motile sperm per ejaculation, so this slight decline in sperm quality should not deter anyone who is considering sperm freezing. A minimum of just 10 million motile sperm is ideal for achieving a pregnancy through intrauterine insemination, so sperm that has been cryopreserved is likely to still be usable if it was within normal parameters to begin with.
In fact, some experts have pointed out that surviving sperm in a thawed sample may be inherently healthier, and may actually be at an advantage and more likely to result in a pregnancy when used in assisted reproductive technology.
While most traditional, brick-and-mortar clinics and labs provide a post-thaw analysis when you opt for sperm freezing, Legacy is the only at-home freezing kit that includes a post-thaw analysis.
Post-thaw analysis is considered an essential step in the sperm freezing process and allows clients to make empowered choices about whether or not to freeze their sperm long-term, how much sperm they should freeze, and which fertility treatment options are open to them. In many ways, it frames the sperm freezing process for clients.
Who should consider sperm freezing
There are many reasons a person might want to consider sperm freezing. From undergoing a treatment that may harm your fertility to simply not being ready for kids just yet, here are the top reasons you might consider sperm freezing:
- You are not ready to have a child — or you’re simply not sure — but you want to preserve your sperm while it is still healthy and viable.
- You’re considering a vasectomy.
- You are about to undergo cancer treatment, like chemotherapy, which is known to reduce fertility. Learn more about fertility preservation for cancer patients.
- You have a low sperm count and/or are preparing for assisted reproductive technology like IVF or IUI.
- You are a trans person about to undergo gender-affirming hormone therapy. Learn more about fertility preservation for trans women.
- You are in a high-risk profession, such as the military or police force, or you spend long periods apart from your partner. Learn more about fertility preservation for the military.
- You are considering being a donor to another couple or individual.
Sperm is healthiest between the ages of 20 and 25. Sperm quality decreases with age, and after age 40, fertility may be significantly lower — and chances of health impacts on the child significantly higher. Ultimately, anyone who produces sperm may consider sperm freezing to safeguard against any potential hazards that may affect their fertility chances down the line.
Sperm freezing costs
Sperm freezing costs depend on a number of factors, such as whether you use a clinic or at-home sperm freezing kit and what your insurance covers. In most cases, there is one cost for sperm collection and analysis, and then ongoing sperm storage costs for your frozen sperm.
At traditional labs, these sperm storage costs can be up to $1,000 per year, and insurance may not cover sperm storage if it’s not deemed medically necessary.
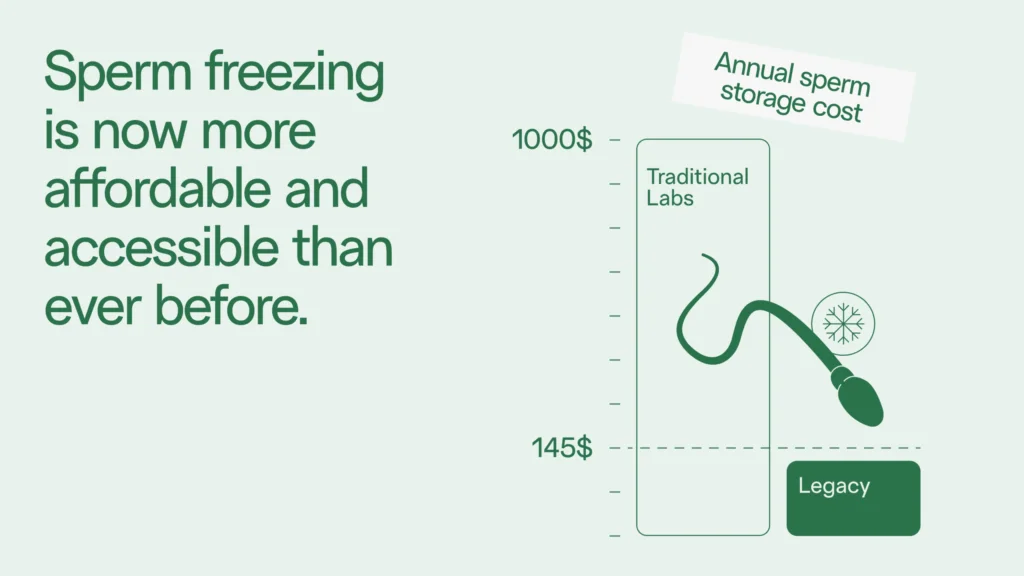
Legacy offers flexible sperm storage options with annual, 5-year, and lifetime plans starting at $245 per year. There are also multiple bundled sperm storage packages, which include semen analyses, cryostorage, and access to fertility advisors, who can help you with these crucial steps in the family-building journey.
What about the cost of post-thaw analysis? At Legacy, post-thaw analysis is always included if you plan to, or may decide to, freeze your sperm — with no extra charge.
Learn more about how at-home sperm freezing kits work in our sperm freezing FAQs.
Find what's right for you






