Male fertility after age 35: What changes (and what doesn’t)?

The myth that only women have a biological clock is misleading, but the research tells a more nuanced story. Male fertility after 35 does change, even if it doesn’t come with the age cutoffs often associated with female reproductive aging.
More American men are becoming fathers later than ever before: the average paternal age at birth rose from 27.4 years in 1972 to 30.9 years in 2015, and fathers over 40 now account for nearly 9% of all U.S. births.1 In cities like New York and San Francisco, first-time fathers in their mid-to-late 30s are increasingly the norm. In today’s world, understanding what’s actually happening to your fertility is the first step toward making informed decisions about family planning.
Key takeaways
- While testosterone declines gradually with age, sperm production continues throughout a man’s lifetime.
- Looking at sperm quality by age shows measurable declines in motility, morphology, and DNA integrity, particularly after the age of 40.
- The underlying mechanisms of advanced paternal age risks for offspring (including associations with autism spectrum disorder and schizophrenia) are still being studied.
- Sperm freezing in your 30s is a practical, proactive option for men who want to preserve their options. This allows you to capture sperm at peak quality before more significant age-related changes occur.
Does male fertility decline with age?
The short answer is yes, but slowly. Unlike females, who are born with a finite number of eggs, men produce new sperm continuously throughout their lives. How long are men fertile? Biologically speaking, indefinitely. Men in their 60s, 70s, and beyond have fathered children. But continuous sperm production doesn’t mean unchanging quality.
A large-scale systematic review and meta-analysis drawing on nearly 94,000 men from 90 studies found consistent age-dependent declines in semen volume, total sperm count, motility, progressive motility, and normal morphology.2 These changes tend to begin gradually in the early-to-mid 30s, with more pronounced effects appearing after 40.

How sperm production changes with age
The process of producing new sperm is called spermatogenesis. This process takes approximately 72–74 days and yields roughly 100 million new sperm per day in healthy younger men.2 The process continues into old age; it’s rare to see a complete stop of sperm production even in elderly men. However, the quality and characteristics of that production change over time.
Semen quality is measured using a few metrics, called “parameters.” These include:
- Semen volume, the amount of semen that’s produced during one ejaculation
- Sperm concentration, the quantity of sperm per mL of semen
- Sperm motility, the percentage of sperm that are moving or “swimming”
- Sperm morphology, the percentage of sperm with the proper size, shape, and structure
- DNA fragmentation, the percentage of sperm that contains damaged or fragmented genetic material
A study analyzing sperm quality across 6,805 samples from men aged 20–63 found that sperm motility peaks before age 30 and declines noticeably after 35, with the most pronounced decrease in men over 40.5 Semen volume also tends to decrease with age, while morphological defects increase. One large analysis suggests approximately a 0.2–0.9% reduction in normal sperm morphology per year.4 Men over 50 have a four-time higher likelihood of morphological abnormalities compared to younger men.4
Importantly, an increase in sperm concentration (the number of sperm per milliliter) may actually be observed in older men, largely because total semen volume decreases. More concentrated sperm doesn’t necessarily mean better; volume and motility still matter for fertility. For others, sperm concentration may decline up to 2.6% year over year.
For a deeper look at how these changes translate across specific age brackets, see our detailed resource on age and male fertility.

DNA fragmentation and mutation rates
Concentration, motility, and morphology are generally the main parameters used to test sperm quality. However, there may also be a change happening at the genetic level of the sperm.
Sperm DNA fragmentation refers to breaks or damage within the genetic material packaged inside each sperm cell. This damage doesn’t show up on a standard semen analysis, but it can significantly affect fertilization success, embryo quality, and pregnancy outcomes.
A systematic review on advanced paternal age (APA) and DNA fragmentation found consistent evidence that DNA fragmentation increases with male age. Most researchers now favor age 40 as the threshold after which this increase becomes clinically significant.6 A separate study found that men aged 40 and over had more than double the risk of having a sperm DNA fragmentation index (DFI) above the threshold associated with declining fertility, compared to younger men.7
Additionally, as men age, their sperm accumulates de novo mutations, spontaneous genetic errors not inherited from either parent. These genetic errors collect in sperm at roughly 3–4 times the rate they do in eggs, and this rate increases with paternal age.9
In short, sperm from older men — especially over 40 — is less genetically healthy than younger men’s sperm, potentially impacting fertility and the health of their future children.
Advanced paternal age and offspring health
One of the more discussed aspects of advanced paternal age risks involves the potential link to neurodevelopmental conditions in offspring, particularly autism spectrum disorder (ASD) and schizophrenia. The concern is grounded in real data, but deserves careful interpretation.
Multiple epidemiological studies have found that children of older fathers have higher rates of ASD. A Danish population study that children of fathers over 39 were 68% more likely to be diagnosed with ASD, compared to children of men in their 20s.8
The relationship between paternal age and schizophrenia is less clear-cut. While schizophrenia risk is increased in older fathers, some researchers have noted schizophrenia risk patterns don’t necessarily follow the accumulation of de novo mutations. This could suggest that different underlying health factors may be at play.10
A rigorous population genetics analysis found that de novo mutations likely account for 10–20% of the increased for ASD or schizophrenia risk in children of older fathers, while another 50% attributed to inherited genetic factors (men with certain heritable traits associated with these conditions may naturally tend to father children later).9
In short, the risk increase from delayed paternity is real but small. As Legacy scientific advisor and Stanford researcher Dr. Michael Eisenberg has described it, the risk increase from advanced paternal age is something like buying two lottery tickets instead of one — your chances go up, but you’re still very unlikely to win.1 This is not a reason to panic, but more so a reason to be informed and plan ahead.
Testosterone decline vs. sperm production
It’s worth separating two things that often get conflated: testosterone levels and sperm production. They’re related, but they don’t age in the exact same way.
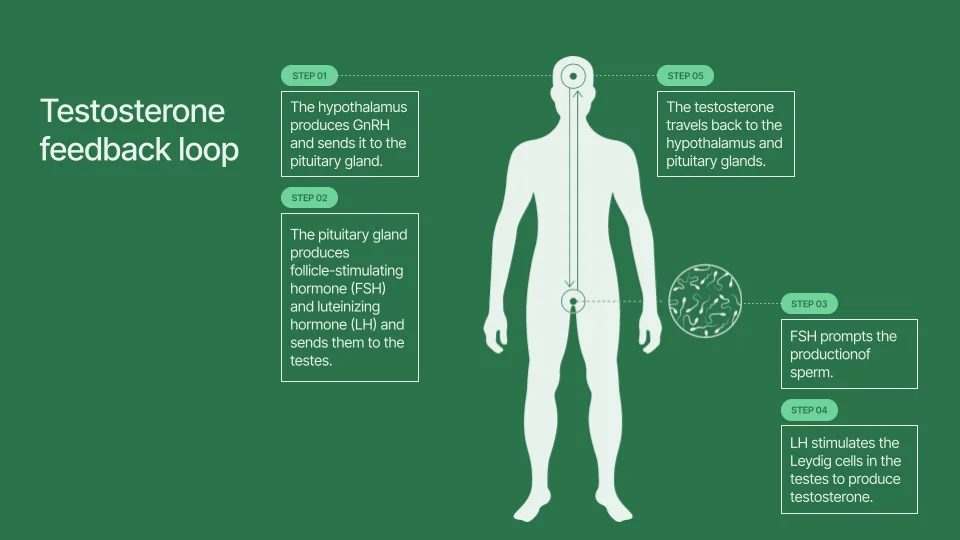
Beginning around age 35, there are changes in the hypothalamic-pituitary-gonadal (HPG) axis, a group of glands and hormones that regulate testosterone production. The HPG axis works like so:
- The hypothalamus in the brain releases GnRH, a hormone that stimulates the pituitary gland.
- The pituitary gland releases luteinizing hormone and follicle-stimulating hormone, two hormones that travel to the testes and drive sperm and testosterone production.
- The testes produce testosterone which travels in the bloodstream back to the hypothalamus, giving the body feedback on how much testosterone is needed.
After 35, men see a decrease in GnRH, which has a chain reaction throughout the axis. Plus, as men age, the testes become less responsive to luteinizing hormone.3 The result is less testosterone produced in the testes.
Testosterone levels decline modestly but measurably with each decade. Some studies also note that men aged 50–76 may experience up to a 50% reduction in the testosterone-producing cells in the testes compared to younger men.4 However, it’s worth noting that lifestyle factors like obesity, sedentary behavior, and chronic disease often account for more testosterone decline than chronological age alone.
So, how does male fertility change after 35?
Male fertility doesn’t just fall off a cliff at 35, but it also doesn’t mean that sperm doesn’t change. Testosterone declines gradually, sperm motility and morphology tend to worsen over time, DNA fragmentation rises after 40, and the risks associated with advanced paternal age are real. Does male fertility decline? Yes, slowly and partially. How long are men fertile? Biologically, for a very long time, but quality and certain offspring-health considerations shift with each decade.
After age 35:
- Sperm motility declines significantly year-over-year, having a potentially significant impact on male fertility
- Sperm morphology also declines substantially with each year of age
- Sperm begin to become less genetically healthy, accumulating fragmentations and de novo mutations each year
- The risk for infertility increases
- The risk for certain health outcomes increase in offspring
- Testosterone levels begin to decline
American men are waiting longer to have children
Why does this matter? Because paternal age is on the rise. The demographic shifts here are striking. Analyzing 168 million U.S. births from 1972 to 2015, researchers found that mean paternal age rose from 27.4 to 30.9 years; with college-educated fathers averaging 33.3 years at their child’s birth.1 The share of newborn fathers over 40 doubled from 4.1% to 8.9% over that same period.1
Geography also matters. Men in Northeastern states and major metro areas become fathers later, on average, than those in the South or Great Plains. In cities like New York and San Francisco, women are conceiving their first children at an average age of 31–32, and first-time fathers in those cities are similarly delayed.11 Men with postgraduate degrees have a mean age at first birth of 32.3, compared to 23.9 for those without a high school diploma.12
These trends show no sign of reversing. As careers lengthen, partnerships form later, and assisted reproductive technology expands reproductive windows, the average age at which American men become fathers will likely continue to rise. That makes understanding the fertility landscape in your 30s and 40s not just personally relevant, but a broader public health conversation worth having.
Learn more: How old are American fathers?
What you can do: Sperm freezing as a proactive move
If you’re a man in your mid-to-late 30s who isn’t ready to have children yet, or who simply wants to preserve future options, sperm freezing offers a concrete solution. Frozen sperm is essentially locked in time, so sperm banked at 33 retains the quality of a 33-year old’s sperm, regardless of when it’s used.
Given what the research tells us about sperm quality by age (declining sperm motility after 35, increasing DNA fragmentation after 40, higher rates of morphological abnormality) freezing sperm in your 30s is a way of getting ahead of those changes before they accumulate. It’s especially worth considering for men who:
- Plan to delay fatherhood until their 40s or beyond
- Are about to undergo medical treatments (chemotherapy, radiation, certain medications) that may affect sperm production
- Have a family history of early male fertility decline
- Simply want the peace of mind of knowing their options are preserved
Legacy makes the process easy and accessible. At-home sperm testing and freezing kits remove the clinic visit from the equation entirely, with lab-grade analysis and long-term secure storage. Whether you’re actively trying to conceive or just thinking a few years ahead, knowing where your fertility stands today is always useful information.
References
1. Khandwala YS, et al. “The age of fathers in the USA is rising: an analysis of 168,867,480 births from 1972 to 2015.” Human Reproduction, 2017.
2. Johnson SL, et al. “Consistent age-dependent declines in human semen quality: a systematic review and meta-analysis.” Ageing Research Reviews, 2015.
3. Ye Y, et al. “Age-related testosterone decline: mechanisms and intervention strategies.” Reproductive Biology and Endocrinology, 2024.
4. Peña FJ, et al. “Age-related decline in behavior and reproductive health in male mice.” Scientific Reports, 2025.
5. Huang Z, et al. “Increasing age in men is negatively associated with sperm quality and DNA integrity but not pregnancy outcomes in assisted reproductive technology.” Frontiers in Aging, 2025.
6. Horta F, et al. “Advanced Paternal Age and Sperm DNA Fragmentation: A Systematic Review.” Aging (Albany NY), 2021.
7. Rosiak-Gill A, et al. “Age-related changes in human sperm DNA integrity.” Aging (Albany NY), 2019.
8. Taylor JL, et al. “Paternal-age-related de novo mutations and risk for five disorders.” Nature Communications, 2019.
9. Janecka M, et al. “Advanced paternal age effects in neurodevelopmental disorders—review of potential underlying mechanisms.” Translational Psychiatry, 2017.
10. Del Giudice M, et al. “Opposite differential risks for autism and schizophrenia based on maternal age, paternal age, and parental age differences.” Evolution, Medicine, and Public Health, 2016.
11. Legacy. “Parental age on the rise in US cities.” givelegacy.com. 12. Schweizer VJ. “30 Years of Change in Men’s Entry into Fatherhood, 1987–2017.” National Center for Family & Marriage Research, 2019.
Find what's right for you






