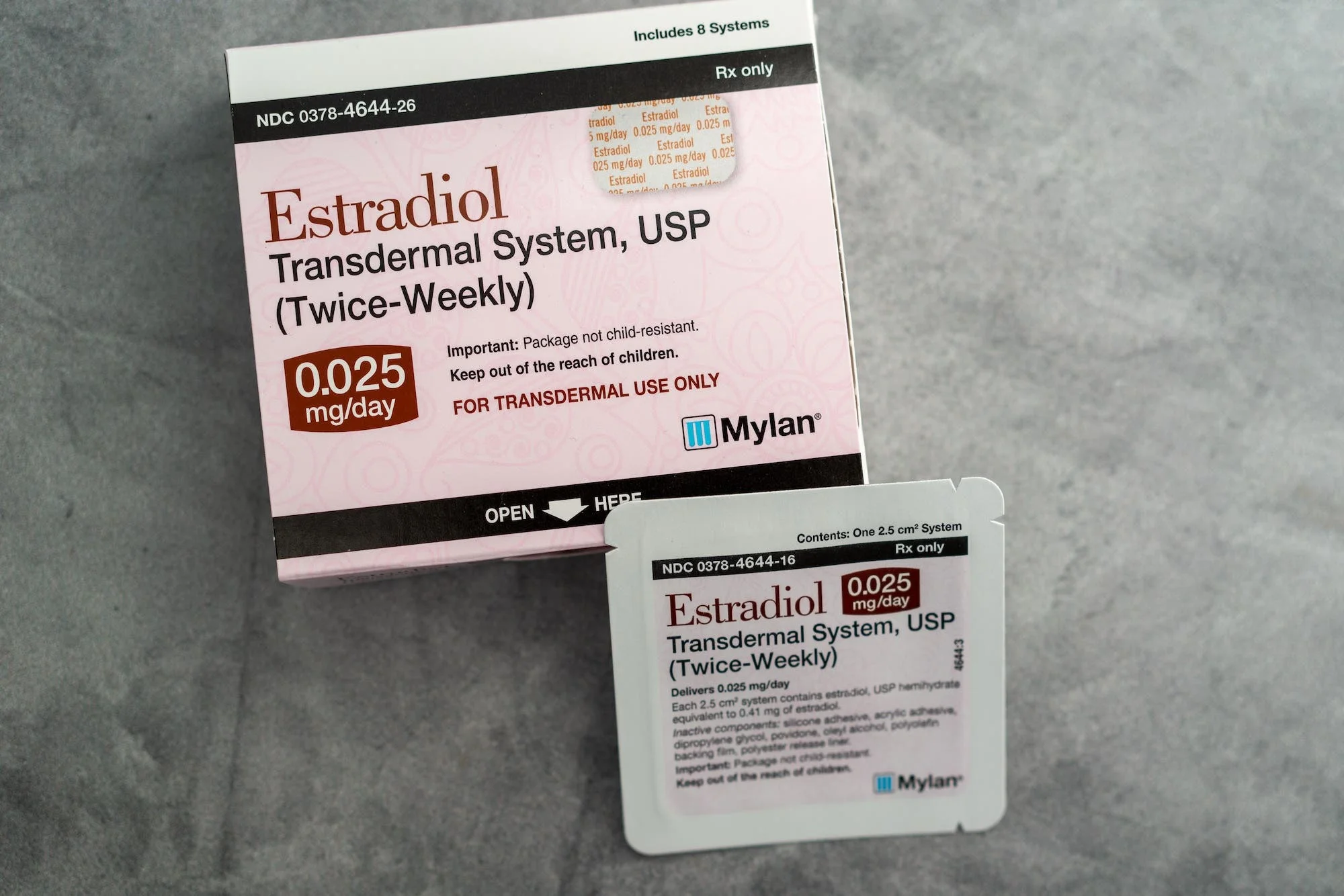
THE SPERM REPORT: Legacy & Carrot survey reveals hormone therapy patients aren’t being informed about fertility risks
Access to hormone therapy is on the rise, yet education about the long-term impact on fertility is not keeping pace. Learn more about fertility preservation options.
We all understand, to some degree, that our hormones play an important role in fertility. But it turns out we’re less informed about how adding hormone supplementation — such as testosterone or estrogen — may impact our ability to have kids.
We conducted a survey of nearly 3,000 respondents to identify gaps in fertility knowledge, and when it came to hormone therapy, the gap was wide. Are those taking testosterone replacement therapy or gender-affirming hormone therapy getting the information they deserve about potential fertility risks?
In this article, we’ll discuss common beliefs about testosterone uncovered by the 2023 Sperm Report that may have led to misinformation about testosterone’s role in male-factor fertility. We’ll also explore how testosterone replacement therapy impacts fertility, and how to plan for the future if you’re considering gender-affirming hormone therapy.
Findings from the 2023 Sperm Report
- Most people do not understand the role testosterone plays in sperm production and are not aware of the impact it has on fertility.
- Taking external testosterone to treat hypogonadism can lead to temporary or long-term infertility for many individuals.
- Individuals in the trans community should receive fertility counseling prior to beginning gender-affirming hormone therapy in order to have a seamless transition.
Legacy and Carrot’s survey
At Legacy, we work with hormone therapy patients daily — both those on testosterone replacement therapy (TRT) for low testosterone, and those taking estrogen and/or androgen-blockers as part of their gender transition. We know from our interactions with these patients that many have not been fully informed about the potential effects on their fertility, but we wanted to dive deeper.
In November 2022, we sent out a survey asking individuals to identify the factors that impact sperm health. We received 2,983 responses from respondents between the ages of 18 and 65. Of the group, 50% identified as cisgender men, 48% as cisgender women, and 2% as trans or nonbinary.* These were our findings.
*Note: when we refer to “women” and “men,” we include all people who self-identify as such.
Misconceptions about testosterone abound
Associations between testosterone, masculinity, and virility are abundant in everyday discourse. Many assume that infertility goes hand-in-hand with low testosterone levels — often referred to as “hypogonadism” in medical speak — and that taking testosterone can improve fertility.
Having low testosterone levels may lead to sexual dysfunction and a reduced libido. However, only a small amount of testosterone is actually required for sperm production, and many individuals with low testosterone can produce healthy sperm. It is not guaranteed that individuals with hypogonadism will face male-factor infertility.
Testosterone replacement therapy (TRT) can address the symptoms of low testosterone. However, it can also negatively impact fertility. Injecting exogenous (external) testosterone disrupts the balance of reproductive hormones, bringing sperm production to a halt.
Within four months of being on TRT, 65% of men with previously normal sperm counts were found to have azoospermia (lack of sperm in semen). In most cases, the impact of TRT on fertility is reversible. However, there is no guarantee. For some, it can take up to two years for sperm counts to return to their baseline level. Failure to recover sperm levels is associated with older patients and individuals who have been on TRT for longer periods of time.
Men on testosterone replacement therapy aren’t aware of the impact on their fertility
TRT is on the rise as a trending treatment for symptoms like lack of muscle tone, fatigue, and low sex drive. Online testosterone providers have made it easy and accessible for young men to get their hands on a prescription, sometimes without even requiring testosterone testing beforehand. The combination of ease of access and lack of education is concerning and requires a change in how we talk and think about testosterone when it comes to male fertility.
Public misconception of the impact testosterone treatments can have on fertility was evidenced by our survey data. More than half of respondents believed taking testosterone supplements would improve a person’s fertility. The lack of awareness of the effect testosterone treatment has on fertility could have lasting impact for those interested in having children in the future.
There remains a significant lack of education even among individuals who are on TRT. From our survey, we found that nearly ¾ of men
are not aware of its potential effect on their fertility.
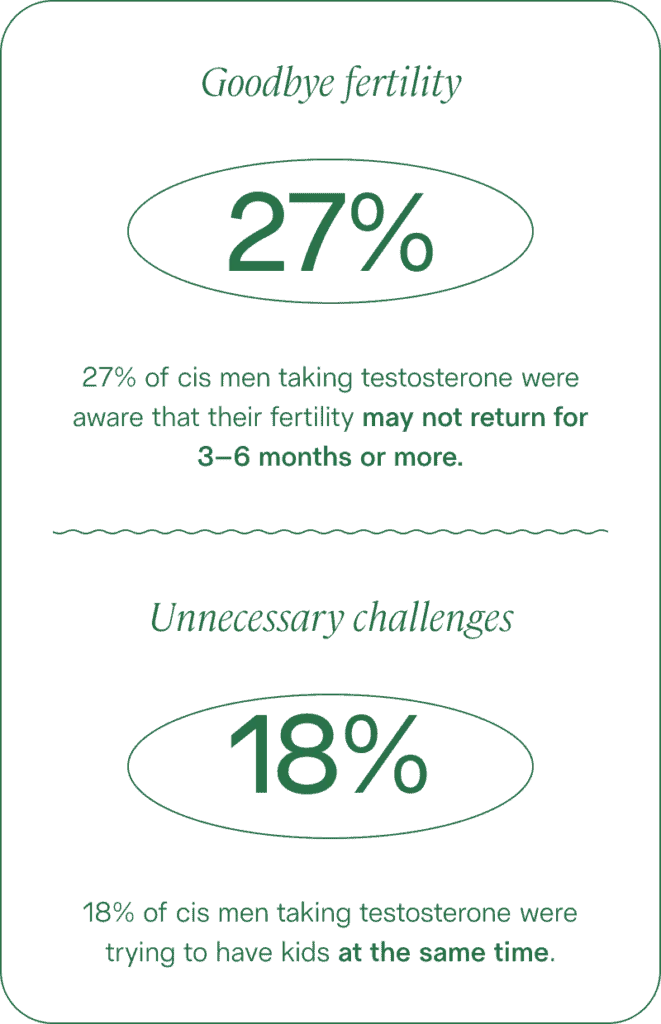
Only 27% of cis men taking testosterone were aware their fertility may not return for three to six months or more. Of those surveyed, 18% of cis men taking testosterone were actually trying for a baby at the same time.
Trans patients on gender-affirming hormone therapy are also lacking information
Medical transition — AKA starting gender-affirming hormone therapy (GAHT) — has been shown to significantly improve mental health for those seeking it. Therefore, increased access to gender-affirming hormone therapy, including virtual care providers, has been hugely net positive for trans patients.
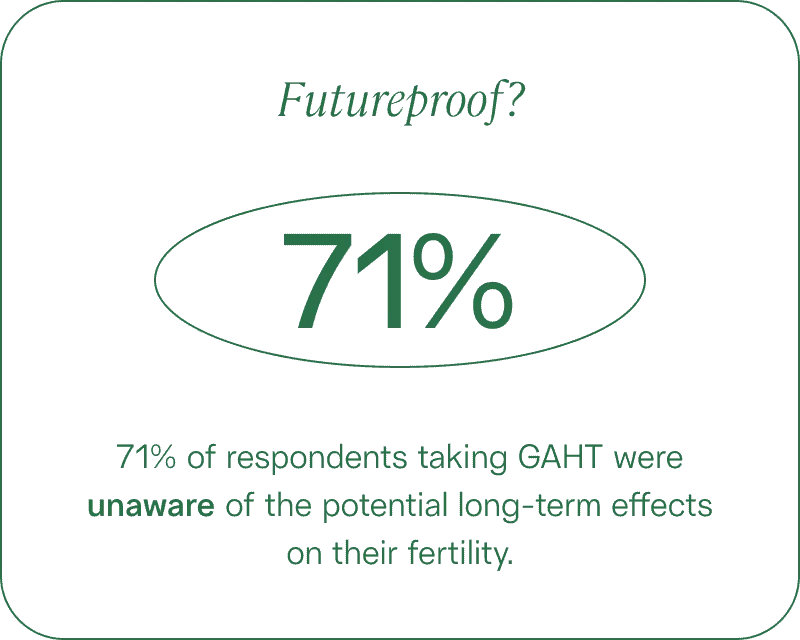
Unfortunately, our research shows that trans women aren’t getting the information they deserve about how their hormone therapy may affect fertility and how to preserve future family-building options. According to our survey, 71% of respondents taking gender-affirming hormone therapy were unaware of the potential long-term effects on their fertility.
How medical transition really affects fertility
Gender-affirming hormone therapy for transgender people with sperm can include estrogen hormone replacement therapy or androgen (testosterone) blocking medication. These hormones are likely to impair fertility, and most trans women taking GAHT will experience a drop or halt in sperm production while taking estrogen or T-blockers.
For some, fertility may recover three to six months after coming off estrogen. However, studies show that 1 in 3 trans women were not able to recover fertility after pausing GAHT. For those who do resume sperm production, sperm concentration may be low and require assisted reproductive technology treatments, like in vitro fertilization (IVF).
Individuals considering estrogen therapy should consider their family planning options — such as sperm freezing — prior to starting hormone therapy, to preserve the healthiest reproductive material.
As trans folks are beginning to transition at younger ages, the impact of hormone therapy on fertility should be an important part of the conversation so that planning and appropriate actions can take place to preserve fertility, if the patient is interested.
Find what's right for you